Home > Medicaid Redetermination
Medicaid renewals and your coverage

If you think you may be at risk of losing health benefits due to Medicaid redeterminations, you have options. Learn more about the process and explore health insurance plans below. We can help you understand how to stay covered.

Medicaid unwinding & redeterminations
During the federal public health emergency for COVID-19, people could keep their Medicaid coverage longer than normal. The continuous Medicaid coverage requirement helped millions of people continue to access the healthcare they needed during the pandemic.
That requirement is now ending because of a change in federal policy and as a result, an estimated 15 million people could lose Medicaid coverage. If your coverage was continued under Medicaid because of the public health emergency, you may now lose coverage if you no longer qualify. But even if you still qualify for Medicaid, you may need to take steps to verify your eligibility.
Medicaid coverage in your state
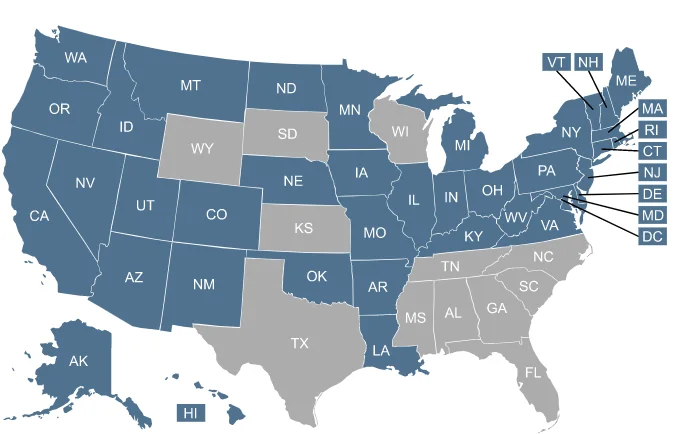
Unwinding of continuous Medicaid coverage will be different in each state. Click your state below to find state-specific information.
Steps to take if you currently have Medicaid
- Update your contact information – Make sure your address and contact information are up to date with the Medicaid department for your state.
- Keep an eye on your mailbox – Carefully read any notices, letters or forms you get in the mail about your Medicaid coverage. Take action and reply promptly to any requests for information.
- Appeal the decision, if necessary – If you receive a notice saying your coverage has been terminated, you may be able to appeal the decision. You may need to provide an account number or a case number.
- Get other coverage – If you no longer qualify for Medicaid, review other coverage options. This may include Marketplace health insurance, an employer plan or Medicare.
(NOTE: The unwinding of continuous Medicaid coverage does not impact the Supplemental Nutrition Assistance Program (SNAP), although the additional pandemic-related SNAP benefits ended in February. And the scheduled end of the federal public health emergency on May 11, 2023, will affect SNAP eligibility for some people. Watch for letters and notices from your state to stay up-to-date on what you need to know about SNAP.)





